Your Medicare Claims Are Getting Denied? Here’s How to Fix That Before It Even Happens!
Let’s be honest. Claim denials are one of the most frustrating and expensive problems in healthcare revenue cycle management. You submit a claim, wait weeks, and then get hit with a rejection that sends your team scrambling to rework everything from scratch. The average cost of reworking a single rejected professional claim runs anywhere from $10 to $25. Multiply that across hundreds of claims a month, and you’re looking at a serious hit to your bottom line.
But here’s the thing, most of those denials are preventable.
The real challenge today is that CMS rules aren’t static. They change. Constantly. Coding requirements shift, coverage determinations get updated, and regulatory guidelines evolve in ways that are genuinely hard to keep up with. Even experienced billing teams find it difficult to stay ahead of all that without the right tools in place.
That’s exactly the problem Micro-Dyn was built to solve.
Why First-Pass Rate Matters More Than Ever
A clean claim submission, one that goes through on the very first attempt, is the gold standard in revenue cycle management. But achieving a first-pass rate above 98% isn’t something that just happens on its own. It requires validating claims before they ever leave your system.
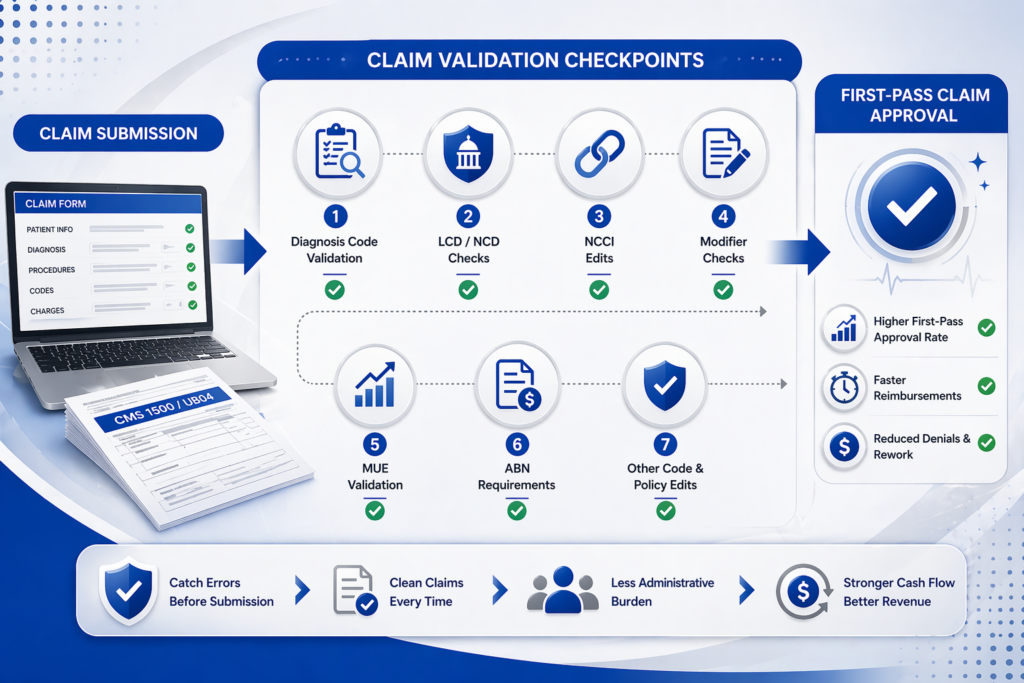
Micro-Dyn’s automated claim-editing solution operates as an API directly integrated into your billing workflow. Before a claim is even submitted to your EDI clearinghouse, the system runs it through a comprehensive set of edits that check for anything that could trigger a downstream denial.
We’re talking about diagnosis code validation, Local and National Coverage Determinations (LCD and NCD), Medically Unlikely Edits (MUE), Correct Code Initiative (NCCI) checks, modifier edits, age edits, Outpatient Code Edits (IOCE), CPT and RVU edits, and Advance Beneficiary Notice of Non-Coverage (ABN) requirements, just to name the highlights. It covers both Professional (CMS 1500) and Institutional (UB04) claim types.
What That Looks Like in Practice
When a claim hits an edit, you’re notified in real time. No waiting 24 days for your clearinghouse to kick it back. No wondering what went wrong. Errors are caught before submission, so your team can make corrections immediately and resubmit quickly.
The result? Fewer denials, shorter days in accounts receivable, and a meaningful reduction in the administrative burden of chasing down rejected claims. You also start catching missed revenue opportunities, situations where claims could have been filed the first time correctly, but weren’t.
One of the features clients appreciate most is that all edits are automatically updated via API. When CMS releases new policies or rate changes, those updates are pushed directly into your system. You don’t have to manually track down what changed or train your staff on new coding initiatives. It just happens.
Setup Is Simpler Than You’d Expect
Getting started with Micro-Dyn’s Medicare editing solution doesn’t require a lengthy implementation process. You configure which edits are turned on or off based on your specific needs, and the system handles the rest. For practices and organizations that want fully automated workflows, the API integration feeds results directly back into your existing billing process.
There are no long-term contracts and no sales people pushing you toward a commitment you’re not ready for. It’s straightforward access to a tool that does exactly what it promises.
If claim denials are cutting into your revenue and slowing down your cash flow, the fix isn’t more staff or more manual reviews. It’s having the right automated system catch problems before they become costly mistakes.
That’s what Micro-Dyn is built for.
